[E-Health #3] All about telecare



This month in “e-Health”, we focuse on telecare. Integrated in 2019 in the French law on the organization and transformation of the healthcare system, it allows remote consultations with pharmacists and medical auxiliaries. It aims to facilitate access to care for all. Find out in this article, everything you need to know about telecare.
Telecare is a care practice carried out remotely thanks to information and communication technologies. It connects a patient with one or more pharmacists or allied health professionals. The patient can choose to be accompanied during the telecare session by a health professional, a caregiver, a family member, etc. Initially, telecare was reserved for certain paramedical professions. With the arrival of the COVID-19 pandemic and the impossibility of consulting health professionals during the lockdown, the practice was extended to new professions. The health crisis highlighted the value of telecare for the French healthcare system, particularly in ensuring continuity of care.
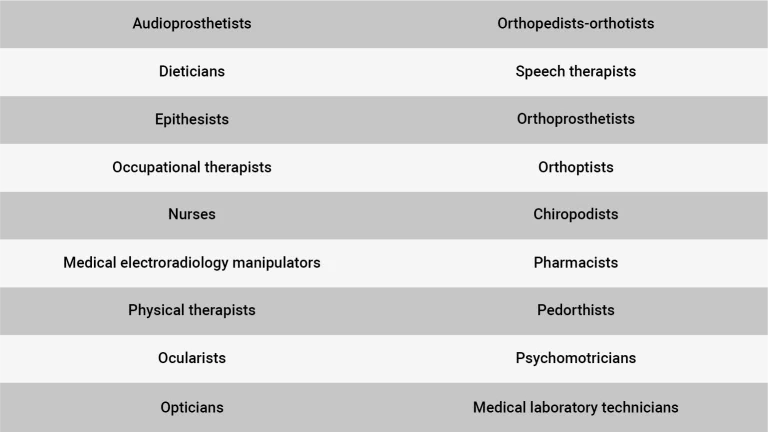
Telecare concerns eighteen different professions in the paramedical field. Here is the list of professionals concerned: audioprosthetists, dieticians, epithesists, occupational therapists, nurses, medical electroradiology manipulators, physical therapists, ocularists, opticians, orthopedists-orthotists, speech therapists, orthoprosthetists, orthoptists, chiropodists, pharmacists, pedicurists, orthopedic pedalists, psychomotricians, medical laboratory technicians.
Telecare is open to all patients.
However, the professional must ensure that the patient is eligible for this practice. To do so, various criteria must be taken into account:
When the care concerns a patient under 18 years of age, the presence of a parent or an authorized adult is mandatory.
The coverage of telecare is similar to a traditional physical consultation. Indeed, the act is billed at the same rate and the terms of reimbursement by the Health Insurance are the same.
Telecare is subject to the professional’s decision and the patient’s consent. In fact, it is a decision shared by both parties. The professional must first judge the relevance of a remote consultation based on the criteria mentioned above. Patient, on the other hand, must give their consent to the telecare procedure. To do this, the professional informs the patient about: the methods of practice of telecare, the materials and equipment used, the possible alternatives, the possibility of being accompanied during the appointment, the protection and security of data, and the methods of coverage and reimbursement. Once the patient’s consent has been obtained, a telecare appointment can be scheduled.
After the appointment is made, the professional will send the patient an invitation with the date, time and connection link. On the day of the consultation, the patient is invited to connect in advance to the appointment and to bring their medical documents (test results, prescriptions, etc.) if useful.
Telecare is performed by video transmission from a smartphone, tablet or computer with a camera. This allows patient and professional identification and a simplified communication. For the session to go smoothly, both the patient and the professional must be in a quiet place that respects the confidentiality of the exchanges. Since they are at a distance, both parties must ensure the quality of the sound and image to facilitate understanding of the medical situation.
At the end of the session, the professional informs the patient about the next steps in their care and any prescriptions. The professional also writes a report of the consultation including the date, time, subjects discussed, prescriptions issued and any other necessary information. This report is recorded in the patient’s file and eventually in the patient’s shared medical file (DMP), if it exists. Finally, the patient can pay for the telecare directly online.

The use of telecare offers many advantages. Firstly, it allows patients to benefit from remote paramedical procedures, thus making their lives easier. This is especially true for people with mobility problems, chronic conditions or busy schedules. It is also an excellent way to fight against “medical deserts” and improve access to care. Secondly, remote consultation reduces the number of trips made by professionals and patients, thus reducing costs, saving time and reducing CO2 emissions. Another advantage is that it makes patients more autonomous and more involved in their health. Finally, it contributes to reducing the length of time patients spend in hospital, and consequently, to relieving hospital congestion.

As with other telemedicine procedures, the French National Authority for Health has defined recommendations for the implementation of telecare. These requirements are intended to provide a framework for the practice and to facilitate the smooth running of remote care. They are similar to those for teleconsultation:
In a report published in February 2021, the French National Authority for Health provides an overview of the professions concerned by telecare. Each profession was asked about the possibility of integrating telecare into their activities. Here are some examples of practices that can be performed remotely.
Pharmacies
For pharmacies, some recurring care activities can be performed via telecare. This allows pharmacists to provide better patient care, to enhance their work and to position them as a health actor. Thanks to real-time video, pharmacists can, for example, conduct pharmaceutical interviews, support patients with chronic pathologies, promote health education or establish shared medication reviews.
Nurses
The French College of Nurses emphasizes its interest in telecare, particularly for care homes and the follow-up of chronic patients. It is also a good tool in rural areas, as it reduces the need for nurses to travel. Several practices can be carried out remotely within the framework of their professions: psychological assistance and support, making, monitoring and renewing non-medicated dressings, collecting observations, monitoring the effects of medication and educating the patient, etc.
Physiotherapists
Telecare allows physiotherapists to alternate physical and remote sessions. This reduces the need to travel, which is an important advantage for patients with chronic diseases. The remote consultation operated thanks to a telecare solution can be used to carry out follow-up consultations, motivational talks, home treatments assisted by connected equipment or even therapeutic education.
Occupational therapists
In the case of occupational therapists, telecare is of interest because it contributes to the continuity of care. Videotransmission is useful to ensure a follow-up of rehabilitation, to support the therapeutic education of the patient, to carry out a follow-up after the delivery of a technical aid (material which allows to compensate an activity limitation), etc.
Dieticians
For the dieticians interviewed, telecare is beneficial for access to care and improving patient follow-up and support. In the context of their activity, it is an interesting tool to carry out consultations at a distance, to visualize the environment and the patient’s lifestyle. It can also improve motivation and avoid dropouts.
Did you like this article? See you next month for a new article on medical response in the context of regulation. In the meantime, don’t hesitate to discover the two articles in the series on teleconsultation and tele-expertise.
Our Apizee Health solution is the perfect answer to the different use cases of telecare. As a 100% web-based remote consultation platform, the solution enables the sharing of medical documents, secure video transmission and billing of the act. Are you looking for a telecare solution? Do not hesitate to contact us to learn more about the solution and our customized support.
Read also:
Claire Boscq, CX Activator and founder of JCX Alliance, shares her unique approach to wellbeing-led customer experience. Discover her vision in this new Apizee CX Voices interview.
[CX Industry Voices] Interview with Claire Boscq
25 Jun 2025
Call Centre Helper’s Xander Freeman spoke to Charles Kergaravat, CMO at Apizee, about the rise of video chat in customer service.
The rise of Video Chat in customer service
20 Jun 2025
Simon Macklin from Salesforce, explains how AI and human empathy combine to shape the future of CX. Discover insights in the latest Apizee CX Voices interview.
[CX Industry Voices] Interview with Simon Macklin
19 Jun 2025
Interested in our solutions?